What do I need to understand about wounds or pressure injuries after severe brain injury?
After a severe brain injury, a person with DoC cannot move their body to relieve the pressure or discomfort that can come from being in one position for a long period of time. And prolonged pressure temporarily cuts off the blood supply to the skin. This can cause damage to the cells, leading to a sore or open area of the skin.
Pressure injuries can happen very quickly, so you need to monitor the condition of your loved one’s skin daily. And keep in mind: skin health can impact overall health.
Immobility is the most common cause of pressure injuries (“bed sores”), and this can occur early while in the hospital and after a person with severe brain injury has gone home and remains immobile. Other factors leading to skin pressure injuries include pressure or rubbing from equipment, moisture from bladder and bowel incontinence, and surgical incisions not healing properly.
Where do wounds or pressure injuries commonly occur?
Pressure-causing injuries often occur on the bony parts of the body that have little padding of muscle and fat:
- Back of the head
- Spine
- Tailbone
- Buttocks
- Shoulder blades
- Side of the hips
- Heels
- Elbows
How do I keep my loved one’s skin healthy?
It is important to check the skin daily to identify and prevent pressure injuries and to make sure the injury does not worsen. Skin care refers to any technique that improves the healing of skin abrasions, blisters, cracks, infections, lacerations, or ulcers. Skin care also includes frequent position changes and management of incontinence to decrease the risk of any skin issue.
Skin care begins in the ICU, it continues through inpatient rehabilitation, and then it continues into the home setting with ongoing support from home-care services. Follow-up can be coordinated with a wound care clinic as needed.
Effective skin care involves the following:
- Providing good daily hygiene to keep skin clean and dry — head to toe
- Providing care to the area(s) involved (e.g., cleaning the wound) as directed by the medical team
- Positioning body parts to avoid pressure and start a turning schedule to prevent new wounds
- Applying compression bandages
- Treating swelling or edema
- Treating infection
- Improving nutrition and blood-sugar levels to promote healing
- Using proper fitting equipment, splints/braces, and cushions
- Improving blood flow and oxygen supply
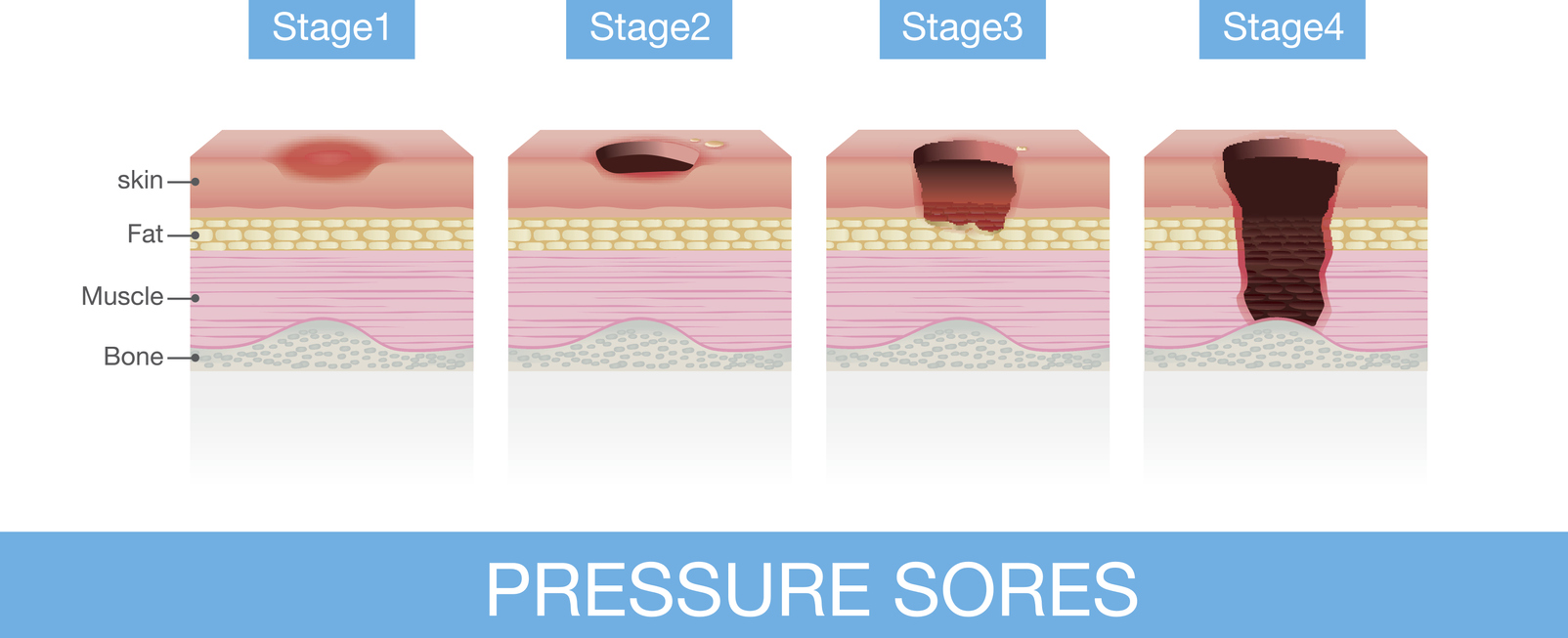
Learn about the stages of skin and pressure injuries in this article from Healthline:
Stages of Pressure Ulcers: Stages, Treatments, and More
From Healthline
For detailed instructions on how to provide good skin care, please explore these PDF guides from Shepherd Center:
Watch how to place padding around your loved one to prevent pressure sores in this video from Shepherd Center:
From Shepherd Center
What do I do if my loved develops wounds or pressure injuries once we're at home?
For open wounds, it is very important to monitor the wound closely and daily to make sure they do not worsen. Pressure injuries can get worse very quickly! First, start with the skin care steps listed above. You will need to stay in contact with your healthcare provider, so that they can recommend the best treatment and monitor concerning areas. Healthcare professionals have training on how to measure the severity and depth of the wound and will develop a treatment plan.
There are also wound-care specialists/nurses who have advanced training to address these issues, so your healthcare provider may consult with them. The goal is to prevent infection and worsening of the problem that can lead to other medical concerns, possibly even surgery.
