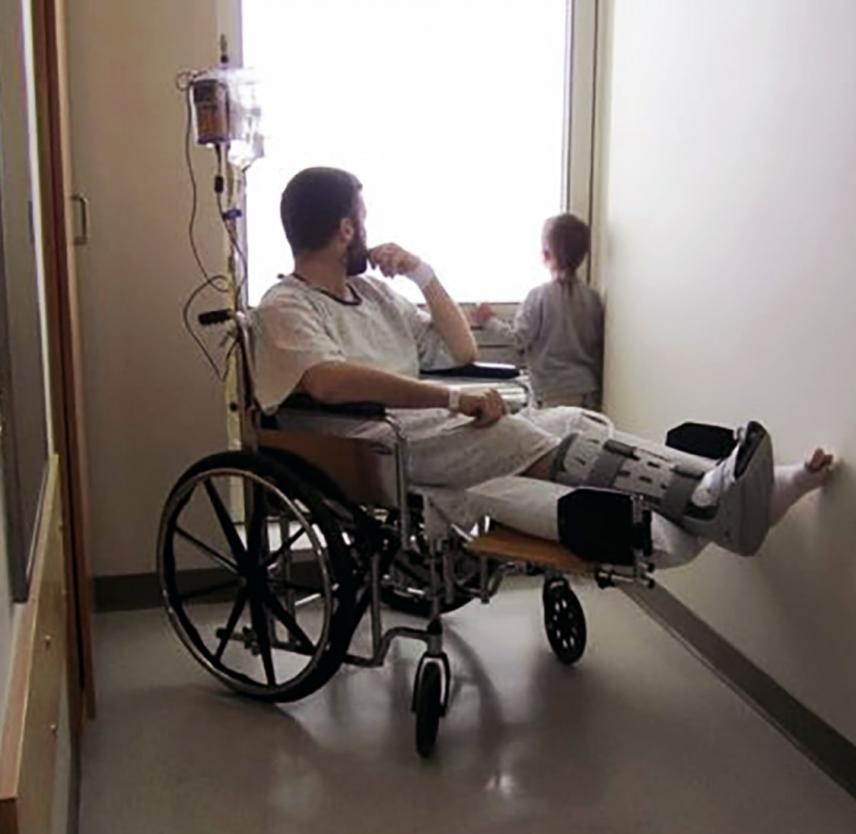
Timothy Bleigh clearly recalls when the bomb went off. The Mine-Resistant Ambush Protected (MRAP) tactical vehicle he was in with five Marines flipped several times through the air before it landed partly on its roof.
“When everything stopped moving, we were just in a pile of gear which was on the bottom of the vehicle… the doors were bent so we couldn’t get out,” he says.
Bleigh, a Navy hospital corpsman, quickly worked to diagnose his injuries.
“I knew right away that both my femurs were fractured. I could move the upper half, but not the lower. I had some visual problems. I knew I got my head banged pretty bad. My back hurt, so I knew I had broken ribs, or a vertebrae,” Bleigh says.
He was near the end of his first tour in Afghanistan, assigned to a Marine personal security detachment, when the improvised explosive device detonated.
“It was a pretty bad situation,” Bleigh says, looking back on that morning. It took him more than a year to recover from the incident and involved multiple surgeries.
Now a newly-commissioned Navy ensign and first-year medical student at the Uniformed Services University of the Health Sciences (USU), Bleigh shares his story and reflects on how his difficult recovery influenced how he approaches patient care.
The video also includes an interview with Dr. Dengler, the director of the Military Traumatic Brain Injury Initiative.
Feeling ‘at home’
Bleigh served as a hospital corpsman for nearly 14 years before coming to USU in 2019 as part of the university’s Enlisted to Medical Degree Preparatory Program, or EMDP2, a program that provides a pathway for enlisted service members interested in a career as a military physician.
Originally from San Jose, Calif., Bleigh started providing care for others after high school when he got a job on a ski patrol team at a resort in Truckee, near Lake Tahoe.
“And I loved it,” he says. “If it paid more, I don’t know that I ever would have changed jobs. I loved every aspect of it and a lot of my coworkers had been either Marines or Navy corpsmen and they had kind of migrated to that job after their service.”
He found the job rewarding, especially when those he helped save came back and expressed what an impact his assistance had made on their lives. But, Bleigh says while in between seasonal jobs and speaking with a recruiter, he decided it felt like the right time to join the military.
“I wanted to continue doing something medical full time, something meaningful… So I joined in 2008, and at that point in time every single person in my [hospital corps school] class was going to field med and going to the Marines to be a ‘greenside corpsman,’ and that’s exactly what I asked for.”
Navy hospital corpsmen are integrated into almost every Marine Corps unit, especially the infantry units — it is part of the medical construct the Navy extends to take care of the Marines, says Bleigh.
“I found that I loved what I was doing,” he says. “I got to live with, train with my neighbors and… I got to work in the clinic every day and break up the monotony of clinic time by going to the field quite often. I always learned something, and I always had something to teach the Marines and it was where I felt at home.”
‘Pretty rough’
So, it was in the field on deployment with the Marines in Afghanistan on March 9, 2011, that Bleigh found himself in the chaotic aftermath of the IED explosion. Despite suffering his own significant injuries in the blast, Bleigh says he was able to find his medical gear and started bandaging the Marines that he could reach. Another corpsman assigned to the Marine personal security detachment climbed in through the turret, which was near the ground, and began removing the injured Marines one by one.
“We didn’t lose anybody, we are very fortunate that we were in a large heavy vehicle rather than a smaller one,” Bleigh says.
He was later medevaced to the Naval Medical Center in San Diego, Calif., for follow-on care and rehabilitation. It was there he was presented with a Purple Heart medal from Marine Corps Gen. Thomas Waldhauser, then the commanding general of the I Marine Expeditionary Forces and U.S. Marine Forces Central Command, for his injuries sustained in the combat theater of operations.
Bleigh was soon attached to the Navy’s C5 program (comprehensive, complex, combat, casualty care) in San Diego for his recovery over the next year and a half.
“That was a blessing. It was kind of its own central facility within a large medical facility, so we had dedicated physical therapists and primary care docs and psychologists and psychiatrists and it helped me get back on my feet quickly,” Bleigh says. “The first year was pretty rough. I broke my right calcaneus, both femurs, three vertebrae, and I had a pretty good concussion, or TBI (traumatic brain injury). The first year or so I had to have several more surgeries to revise, remove, or add bigger hardware.”
He describes that time during his recovery as being on something of a rollercoaster.
“I’d improve a little bit and kind of see a way forward and then have another surgery and have to rewind,” Bleigh says. “But in that journey, I spent a lot of time ‘on the table’ and I spent a lot of time just really picking the brain of my physical therapists and my orthopedists and my corpsmen who were there with us and just really dissected every which way I could find a solution to whatever I was facing that day — because sometimes it was day by day.”
Bleigh says he drew a lot of inspiration from his wife, two young children, and what he calls his “Navy family.”
“They’ve been really important to me throughout the journey,” Bleigh says. “I woke up every day to three living, breathing sources of inspiration to get better.”
It took time, but he was able to pass the Physical Readiness Test and return to active duty.
A ‘wealth of knowledge’
Bleigh says he’s found that his long recovery helped him to relate and empathize with his patients.
“I felt comfortable at the bedside talking to a patient, doing my exams and figuring out what they needed and it occurred to me that I spent so much time ‘on the table’ that I felt comfortable talking to someone also (in that situation),” Bleigh says.
He adds when medical providers are trying to figure out what to do for a patient, and there’s a difficult clinical decision to make, or a decision that they need to decide on due to the monetary cost — his experience provides him with a simple solution.
“I’ve gotten used to just saying ‘hey, if we ask the question: is this the right thing for our patient?’ And we can answer that ‘yes,’ then all the following questions don’t matter,” Bleigh says. “Because we’re afforded the ability to go to whatever lengths we need to do the right thing for our patients.”
Eventually, Bleigh says he decided to seek greater responsibility, and attended the Navy’s prestigious Independent Duty Corpsman (IDC) School for hospital corpsmen.
“It didn’t take very long after IDC school to realize there’s this whole other wealth of knowledge in the realm of medical care that… I guess I was dipping my toe into it and I wanted a lot more,” Bleigh says. “So about six months after I graduated from IDC school, I sort of charted a path to becoming a doctor. I hadn’t started my undergraduate degree yet, so I planned a path to my undergraduate degree and a bridge program to link me from that to medical school.”
That bridge program was USU’s EMDP2, a two-year program at George Mason University that prepares enlisted service members to successfully apply for admission to medical school at USU, or at other U.S. medical schools through the Armed Force Health Professions Scholarship Program. He completed it in May 2022 and started medical school at USU on August 1.
Bleigh says he looks forward to the day when he’s able to help others using his experiences as both a medical care provider and patient.
“I want to spend my time paying that forward because I was afforded so much time and knowledge to help me get better,” he says. “I feel I could use that (experience) to treat my patients.”
The appearance of U.S. Department of Defense (DoD) visual information does not imply or constitute DoD endorsement.
