“Close your eyes and think about the vacation you took on a warm, sunny beach. Now, tell me every detail of what you see, hear, smell and feel.”
- imaginal exposure therapy
“Let’s take a trip to the beach today.”
- in vivo exposure therapy
“Step into this replica of your beach vacation, which you’ll experience with all your senses as if you’re actually there, but I’ll control the environment so you won’t get too hot, too sandy or too uncomfortable overall.”
- virtual reality exposure therapy
We’re not actually going to talk about your beach vacation. These scenarios represent different exposure therapy techniques mental health care providers use to treat patients with posttraumatic stress disorder (PTSD). Substitute war and battlefield for the ideas of vacation and beach in the examples, and you may see that virtual reality exposure therapy may be a more manageable option for service members with PTSD.
While all of the therapies are effective and require patients to confront their traumatic experience in vivid detail, virtual reality exposure therapy takes place in an environment the provider can control — the virtual environment.
Before we talk more about these techniques, it’s important to point out that exposure therapy often starts with learning coping skills, such as ways to relax through deep breathing or meditation. This is part of cognitive behavioral therapy, a short-term therapy that helps restructure unhealthy thinking patterns. A firm foundation here sets the stage for exposure therapy, where patients will work through reactions or feelings they experience in response to traumatic memories and other reminders of a traumatic event.
Let’s look closer at the therapies.
Imaginal Exposure Therapy
If using imaginal exposure therapy, the provider will ask you to close your eyes, picture the traumatic experience, and then talk about it in first person, present tense, like it’s actually happening. The provider will ask for as much detail as possible about what you see, hear, feel and smell.
It sounds simple, but can be very difficult. Reliving the trauma is hard at first, but over time, most patients find it gets easier to talk about it and to engage in activities or situations they had been avoiding. As a result, symptoms tend to lessen and the patient starts to cope with rather than avoid the traumatic experience.
While imaginal exposure therapy works very well for some, many aren’t able to talk in detail about their trauma. The desire to avoid any reminders of trauma is one of the defining features of PTSD. Imaginal exposure therapy puts a lot of pressure on patients to repeatedly describe their trauma in increasingly vivid detail.
In Vivo Exposure Therapy
In vivo (living body) exposure therapy involves repeatedly confronting something you fear, whether it’s an activity, situation or behavior, as long as it’s not dangerous. Over time, the technique can help you feel less fearful and build resilience. In vivo therapy builds confidence to cope with stressful situations. With this technique, however, the provider cannot control the activities, situations or behaviors the patient confronts. Also, there are circumstances not practical for the patient to confront, such as combat trauma, which limits the use of this therapy.
Virtual Reality Exposure Therapy
Virtual reality exposure therapy combines elements of imaginal and in vivo therapies — confronting traumatic experiences in vivid detail, but under circumstances the provider can control.
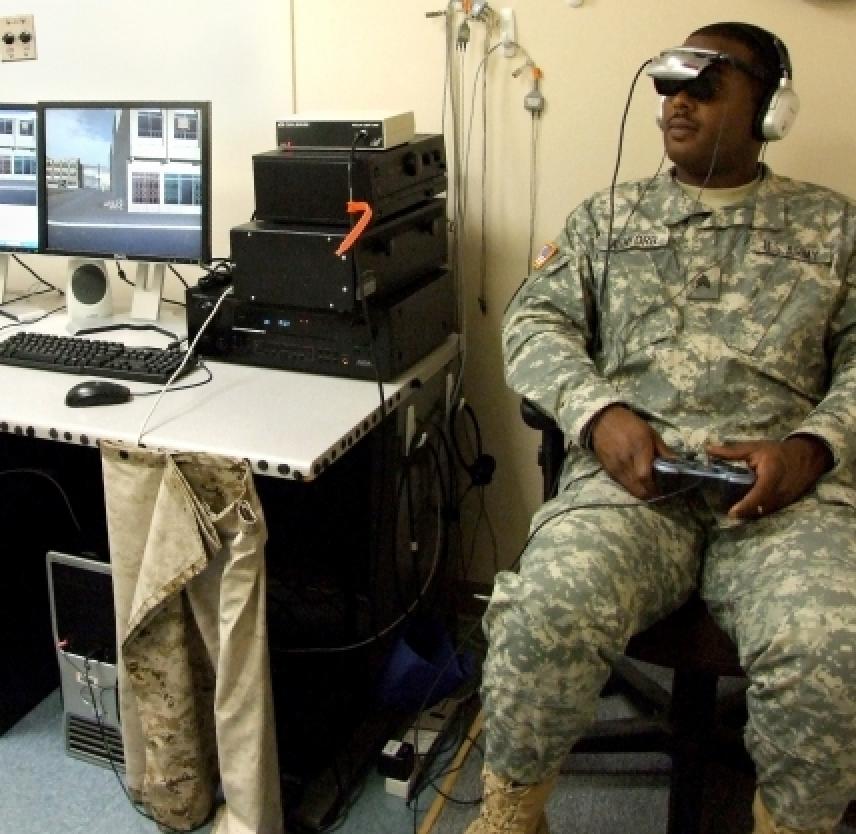
Patients equipped with a head-mounted visual display are exposed to a virtual world in which they experience the sights, sounds and even smells of combat in order to confront their trauma in a safe and controlled environment. With gradual exposure to memories of the traumatic event, the patient is able to deal with emotions the memories bring up.
This technique was first used to treat posttraumatic stress disorder in Vietnam War veterans. The therapy is used to treat a wide range of phobias, including fear of small spaces, flying and heights. Virtual reality exposure therapy is also effective for social phobia or fear of public speaking, and is used to treat addictions to tobacco, alcohol and drugs.
Iraq and Afghanistan Virtual Environment
At Walter Reed National Military Medical Center in Bethesda, Maryland, we use one of the most sophisticated virtual environments ever developed to treat service members from current conflicts with PTSD. Colleagues at Madigan Army Medical Center, Washington, San Diego Naval Medical Center and the Department of Veterans Affairs also use this virtual environment.
Here are some conditions the provider can control:
- The patient can enter the virtual environment at a point far removed from the traumatic event and gradually progress to whatever initiated the trauma.
- The patient can be alone, with a buddy or an entire patrol; walk through an urban environment; be a driver, passenger or sit in the gun turret of a Humvee; transition from the vehicle to proceed on foot.
- The provider can introduce intermittent or persistent machine gun fire, mortars or rocket-propelled grenades, as well as friendly or enemy soldiers, civilians, and air and land vehicles. The provider can also control the weather as well as the time of day or night.
- In addition to sights and sounds, a vibration platform conveys the rumble of a moving vehicle and the feel of an explosion, while a smell machine wafts in odors such as cordite, burning trash, body odor and Middle Eastern spices.
Virtual reality exposure therapy is not necessarily for everyone. It can be daunting for patients to know that they’ll confront virtual scenarios linked to their trauma. However, if used correctly, virtual reality exposure therapy can be powerful and effective for treating PTSD.
The arguments for using exposure therapy are compelling. Research we’ve undertaken at Walter Reed has shown that the brain actually returns to normal after this treatment, including key components involved in the symptoms of PTSD: amygdala, hippocampus and frontal lobe. Further research is needed to see if we can identify who will benefit most from which therapy, based on genetics, cortisol levels (an indication of stress) or other factors.
Used with permission from Dr. Michael Roy, professor of Medicine at Uniformed Services University of the Health Sciences.
Learn more about research like exposure therapy, here.

Comments (1)
Please remember, we are not able to give medical or legal advice. If you have medical concerns, please consult your doctor. All posted comments are the views and opinions of the poster only.
Anonymous replied on Permalink
Exposure therapy represents the very definition of cruel and unusual punishment!