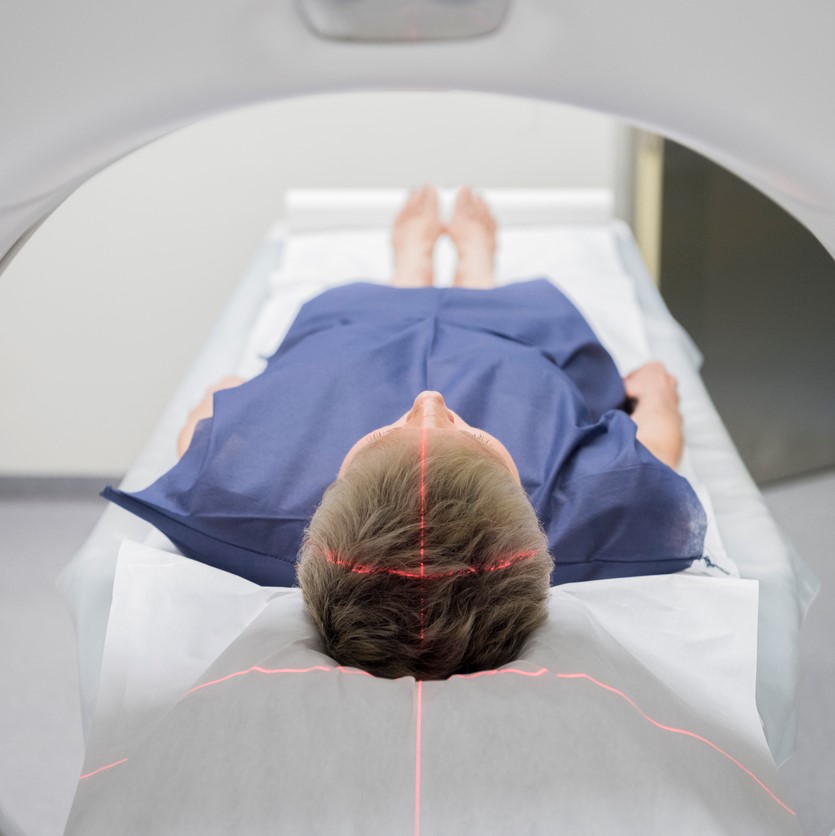
Brain Scans
Neuroimaging—or brain scanning—includes the use of various techniques to either directly or indirectly image the structure, function, or pharmacology of the brain. Brain imaging methods allow neuroscientists to see inside the living brain. These methods help neuroscientists understand the relationships between specific areas of the brain and what function they serve.
Neuroimaging falls into two broad categories:
- structural imaging – deals with the structure of the brain and the diagnosis of large-scale intracranial disease—such as a tumor—as well as injury.
- functional imaging – measures an aspect of brain function, often with a view to understanding the relationship between activity in certain brain areas and specific mental functions. It is primarily used as a research tool in cognitive neuroscience and neuropsychology.
The main types of neuroimaging include:
- Computed Tomography Scan (CT)
- Magnetic Resonance Imaging (MRI)
- Positron Emission Tomography Scan (PET)
- Diffusion Tensor Imaging (DTI)
There is also an emerging technology called Transcranial Magnetic Stimulation (TMS), which is not a type of neuroimaging but is related.
Take a look at these slides and descriptions below to get a better understanding of the use of neuroimaging in the brain.
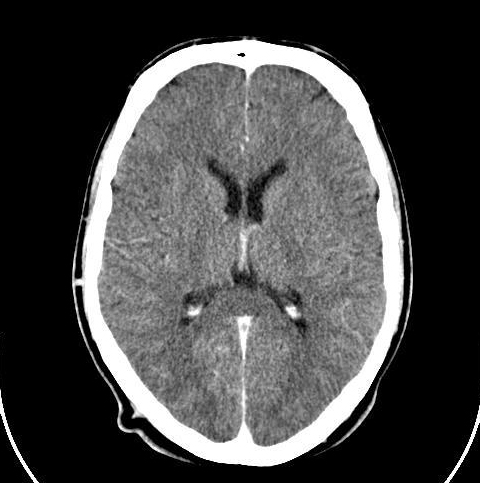
Computed Tomography Scan (CT)
Computed Tomography Scan (CT) scans use a series of X-ray beams passed through the head. The images are then developed on sensitive film. This method creates cross-sectional images of the brain and shows the structure of the brain, but not its function. It is the test of choice to evaluate for the four types of intracranial hemorrhage—subdural, epidural, intracerebral, or subarachnoid, which specifically means bleeding or swelling of the brain during the first 24 to 48 hours after injury. It is also used to detect a skull fracture.
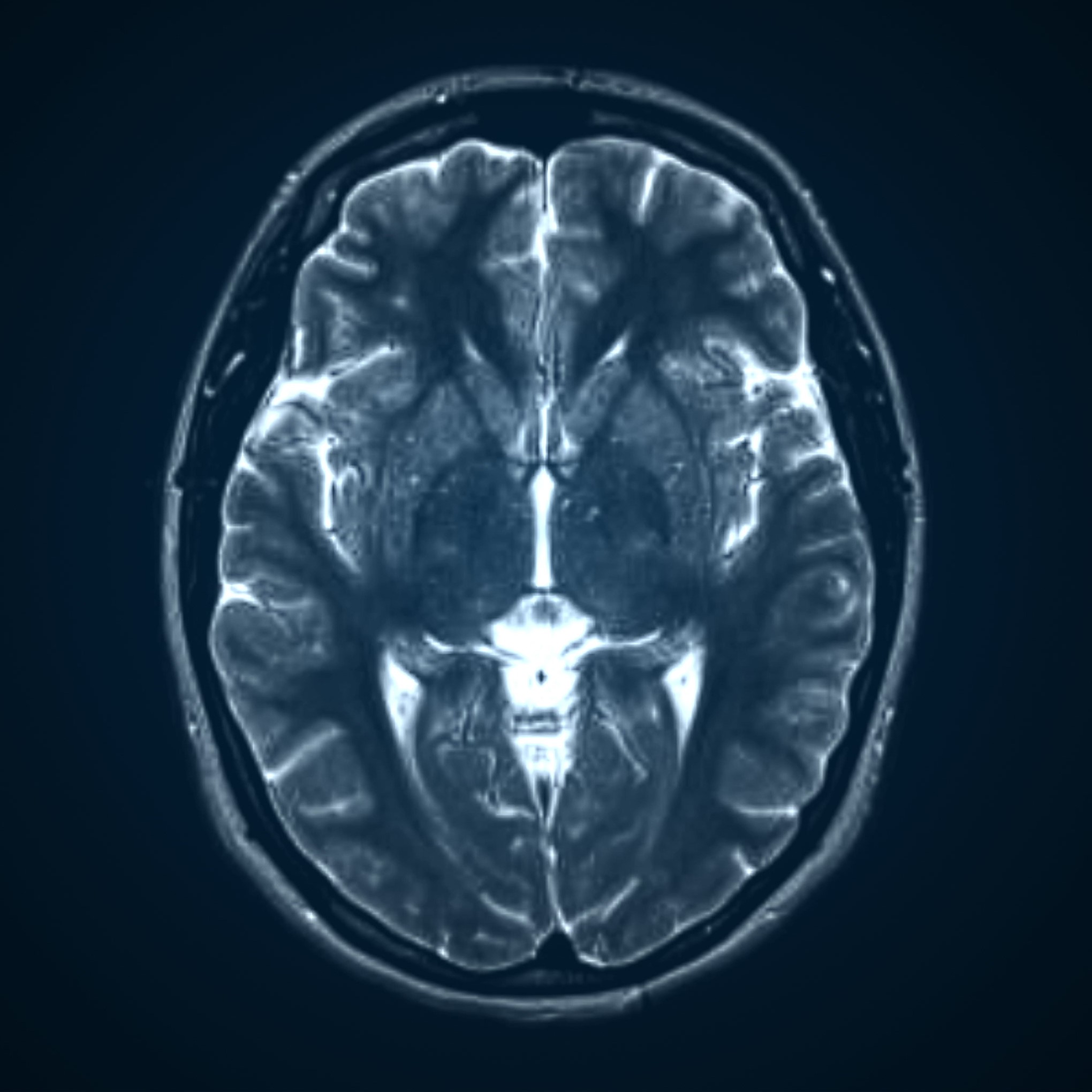
Magnetic Resonance Imaging (MRI)
Magnetic Resonance Imaging (MRI) scans use echo waves to discriminate among grey matter, white matter, and cerebrospinal fluid. These cans can show if there’s a fracture or bleeding. An MRI may be helpful if a person’s symptoms continue for 48 hours or more after the injury, or if symptoms get worse.
“For diagnostic purposes, and even for characterization of the extent of injury, we predominantly rely upon magnetic resonance imaging. This is our standard imaging modality. With an MRI, our standard measures are good at characterizing whether there's been blood, whether there's been a contusion or a bruise to the brain, or whether there is significant damage to axons that actually result in lesions that we characterize in the brain. It's also, of course, very good at tumor, at stroke, at ischemic damage.” — Deborah Little, PhD, professor, Department of Psychiatry and Behavioral Sciences, director of research for the Trauma and Resilience Center, McGovern Medical School, University of Texas
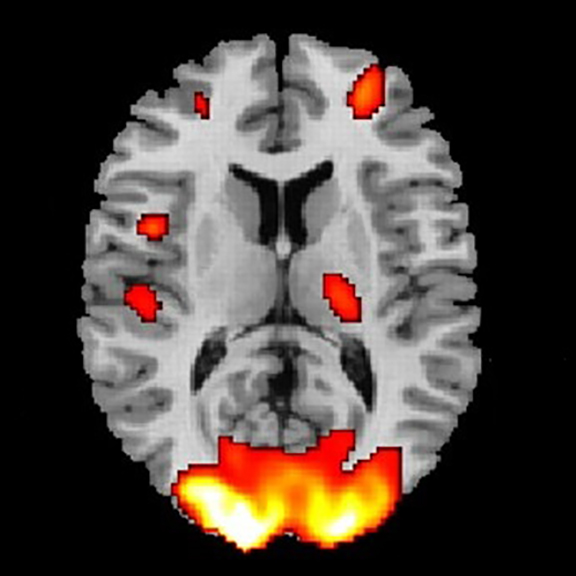
Functional MRI (fMRI)
Functional magnetic resonance imaging (fMRI) scans are a series of MRIs measuring brain function via a computer’s combination of multiple images taken less than a second apart. For this imaging test, doctors ask patients to do something while in the MRI machine like opening and closing their right hand for 30 seconds and then opening and closing their left hand for 30 seconds. Then, the doctors model the change in signal associated with an increase in blood related to that task. So, areas involved in opening the right hand will show increased signal. This allows images to be created that reveal how the brain does tasks. This is potentially useful in brain injury when the brain structures all appear normal but the brain is functioning in a different way. It is important to know that fMRI is not approved for clinical use for diagnosis of TBI.
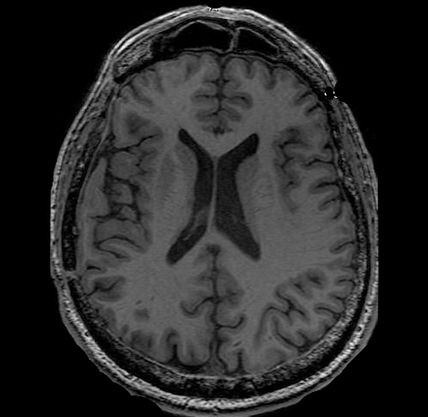
T1-Weighted MRI
The T1-Weighted MRI is the standard imaging test and part of every general MRI exam. It provides doctors with a very clear view of brain anatomy and structure. It can also show damage in brain injury but generally only when the damage is very significant.
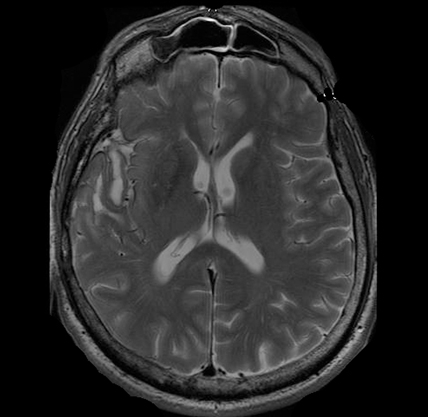
T2-Weighted MRI
The T2-Weighted MRI is also a standard part of every MRI exam. But unlike T1-weighted imaging, the T2 allows visualization of severe diffuse axonal injury such as what is expected following severe TBI. T2-weighted scans are used to measure white matter and cerebrospinal fluid in the brain, as this type of scan is more suited to measure fluid rather than soft tissues.
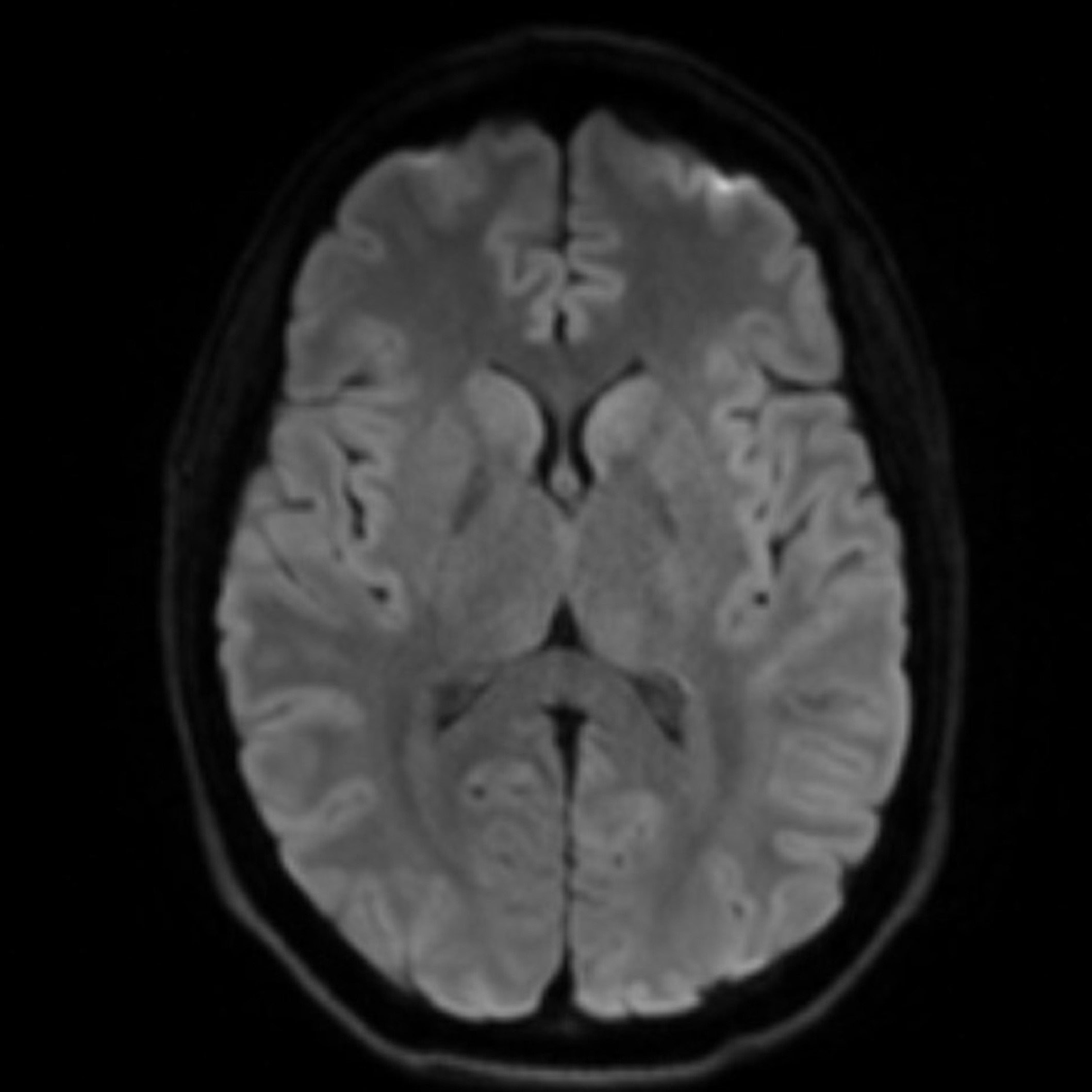
Diffusion Weighted MRI (DWI)
Diffusion Weighted MRI (DWI) shows alterations in tissue integrity— the ability of body tissues to regenerate and/or repair to maintain normal physiological processes. In ischemic injury—such as many types of stroke or when blood is not able to get to all parts of the brain—there is a chemical reaction in the cells. As the cells die because of lack of blood flow (with oxygen), there is an increase in sodium and this changes (increases) the amount of water in the tissue. DWI is very sensitive to this change. In fact, using DWI, doctors can identify a stroke or ischemic injury within seconds of occurrence.
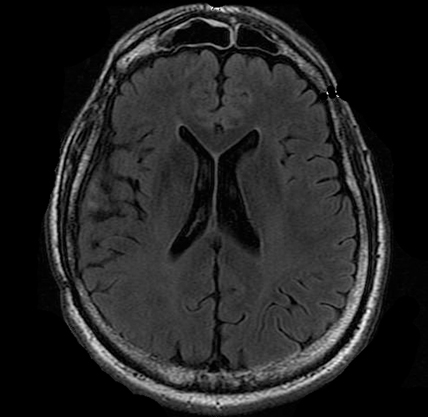
Fluid-Attenuated Inversion Recovery (FLAIR) MRI
Fluid-Attenuated Inversion Recovery (FLAIR) MRI is also sensitive to water content in brain tissue. This is very useful in patients who have reductions in brain tissue following an injury. Most commonly, however, FLAIR is used to visualize alterations in tissue in diseases such as multiple sclerosis.
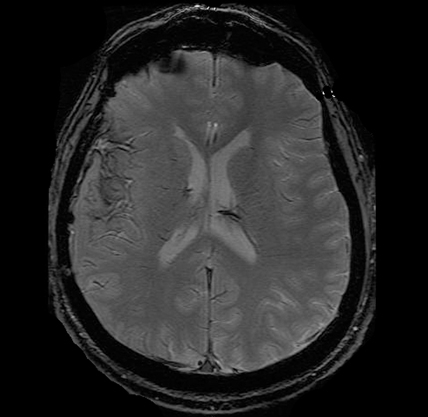
Gradient Record MRI (GRE)
Gradient Record MRI (GRE) shows blood or hemorrhaging in the brain tissue. This is very important in acute brain injury. CT scans are also very useful in this stage but sometimes miss very small bleeds—or so called microbleeds—in the brain. Other types of MRI cannot easily detect these types of injury, so GRE is particularly useful to physicians who suspect these injuries may be present in a patient.
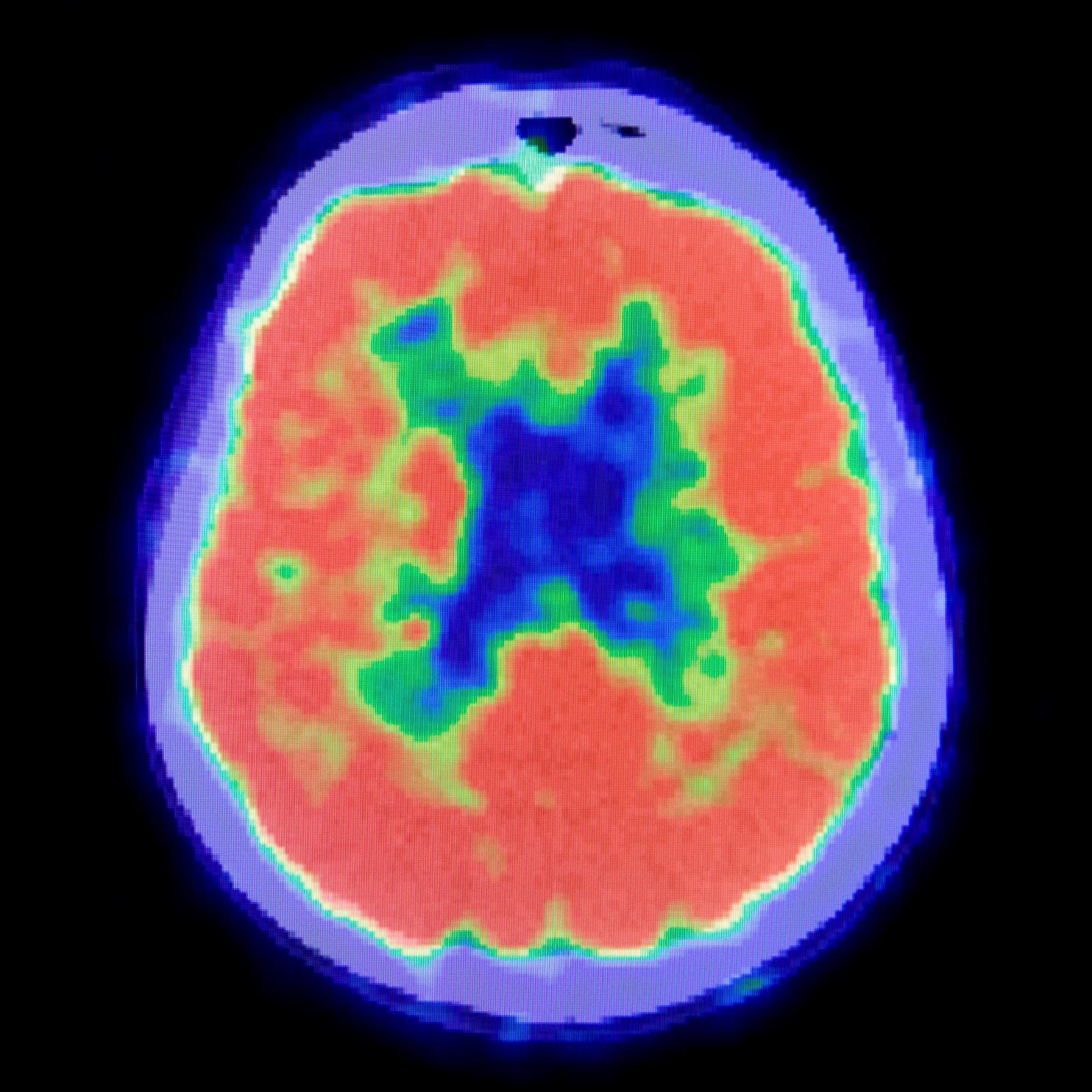
Positron Emission Topography (PET)
Positron Emission Tomography Scan (PET) measures brain metabolism. Different applications of PET allow one to "see" pathology associated with Alzheimer's disease, for instance, that cannot be visualized any other way. Used in a different way, PET also allows doctors to see how different areas of the brain use oxygen or glucose—both very important in understanding not just what the damage might look like but also how the brain provides energy to itself. In brain injury research, PET scans are used to identify how metabolic processes may be changed after a brain injury. For instance, the brain may absorb less glucose (sugar) after a brain injury, which may affect how an individual processes information. PET has recently been used in tandem with MRI to identify (with a high degree of spatial accuracy) specific brain regions that may be experiencing metabolic changes after injury.
“PET scans look at metabolism in the brain. We inject the radiotracer glucose, and the glucose is utilized in the brain, and areas of the brain that use more glucose light up stronger, and areas that use less glucose do not light up as strong. So, we can see areas of the brain that are potentially damaged and not utilizing glucose as much as they should be.” — Gerard Riedy, MD, PhD, neuroradiologist, National Intrepid Center of Excellence (NICoE), Walter Redd National Military Medical Center Bethesda
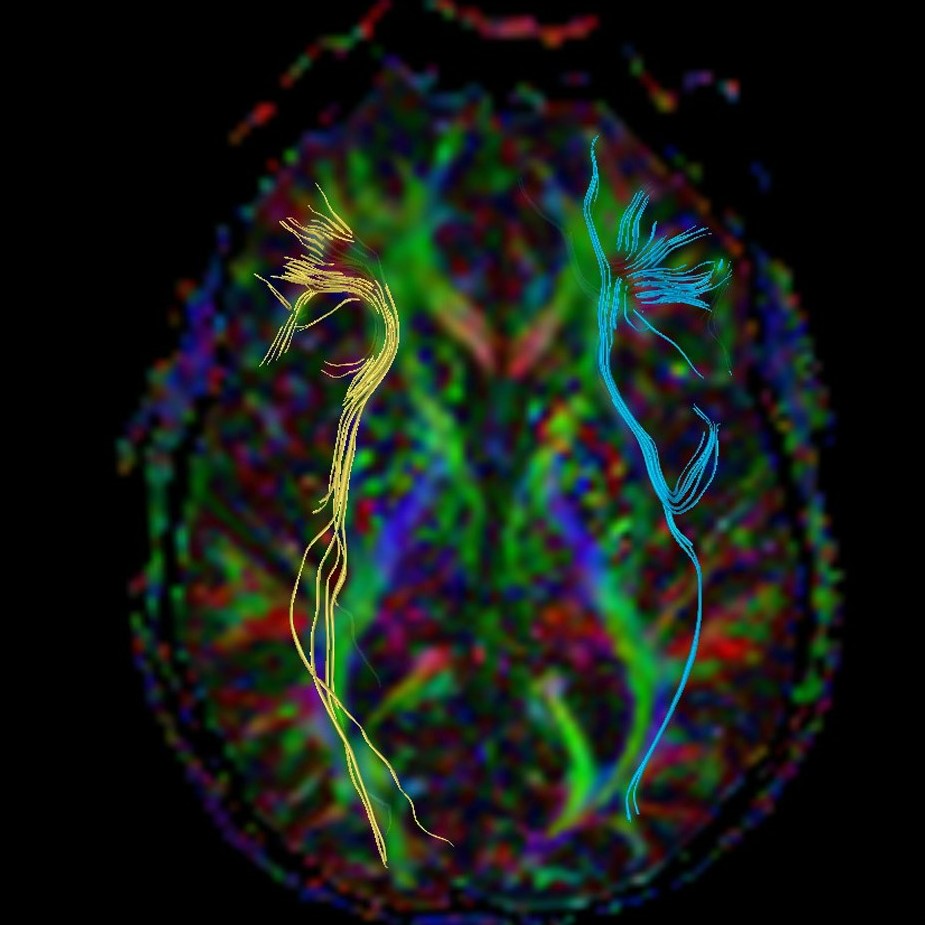
Diffusion Tensor Imaging (DTI)
Diffusion Tensor Imaging (DTI) shows white matter tracts in brain tissue. These tracts allow different parts of the brain to talk to each other. Think of the brain as if it were a computer. With DTI, doctors can see and measure the "cables" connecting parts of the brain. DTI can provide information about damage to parts of the nervous system as well as about connections among brain regions.
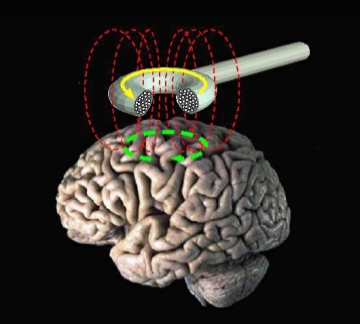
Transcranial Magnetic Stimulation (TMS)
Although not an neuroimaging technique, per se, TMS is an FDA-cleared noninvasive treatment that uses gentle magnetic pulses to activate areas of the brain involved in mental health and addiction conditions. The treatment is well-tolerated, has no systemic side effects.
“Though still in the research stages, TMS may be a useful non-invasive brain stimulation tool to study the effects of targeted TMS treatment on individuals with chronic symptoms after brain injury.” — Cooper Hodges, PhD, Polytrauma Research fellow at the DC VA hospital

Comments (5)
Please remember, we are not able to give medical or legal advice. If you have medical concerns, please consult your doctor. All posted comments are the views and opinions of the poster only.
Anonymous replied on Permalink
Thank you for your specialized information. I recently fell off my step ladder onto concrete and banging the back of my head on the corner of a brick wall. I am fortunate to be here!! I was able to drive to emergency with a bleeding laceration. Had a CT scan, was told it looked normal, needed 4 or 5 staples & Tic shot.
I understand hitting the head in anyway is very serious & dangerous, so I am scared & concerned especially since I'm getting feelings of tightness, which could be the staples, some head pain, some throbbing & when I was talking, couldn't think of a certain word. The accident happened on 8/4/22 & supposed get staples removed Monday, but not sure ready. Will appreciate any feedback. Thank you.
Terri replied on Permalink
Can you describe Progressive Supranuclear Palsy...and which tests would be used to diagnose?
Anonymous replied on Permalink
Anonymous replied on Permalink
Anonymous replied on Permalink